Raising the Bar in Airway Safety: Tracheal Intubation Excellence in the PICU and CICU
Tracheal intubation is a high-stakes procedure for critically ill children. When performed in pediatric intensive care units (PICUs) and cardiac intensive care units (CICUs), the risks — including oxygen desaturation, hypotension and airway trauma — can be life-threatening. At Children’s Wisconsin, our dedicated multidisciplinary team has transformed how these procedures are approached, setting new standards for safety, communication and continuous improvement.
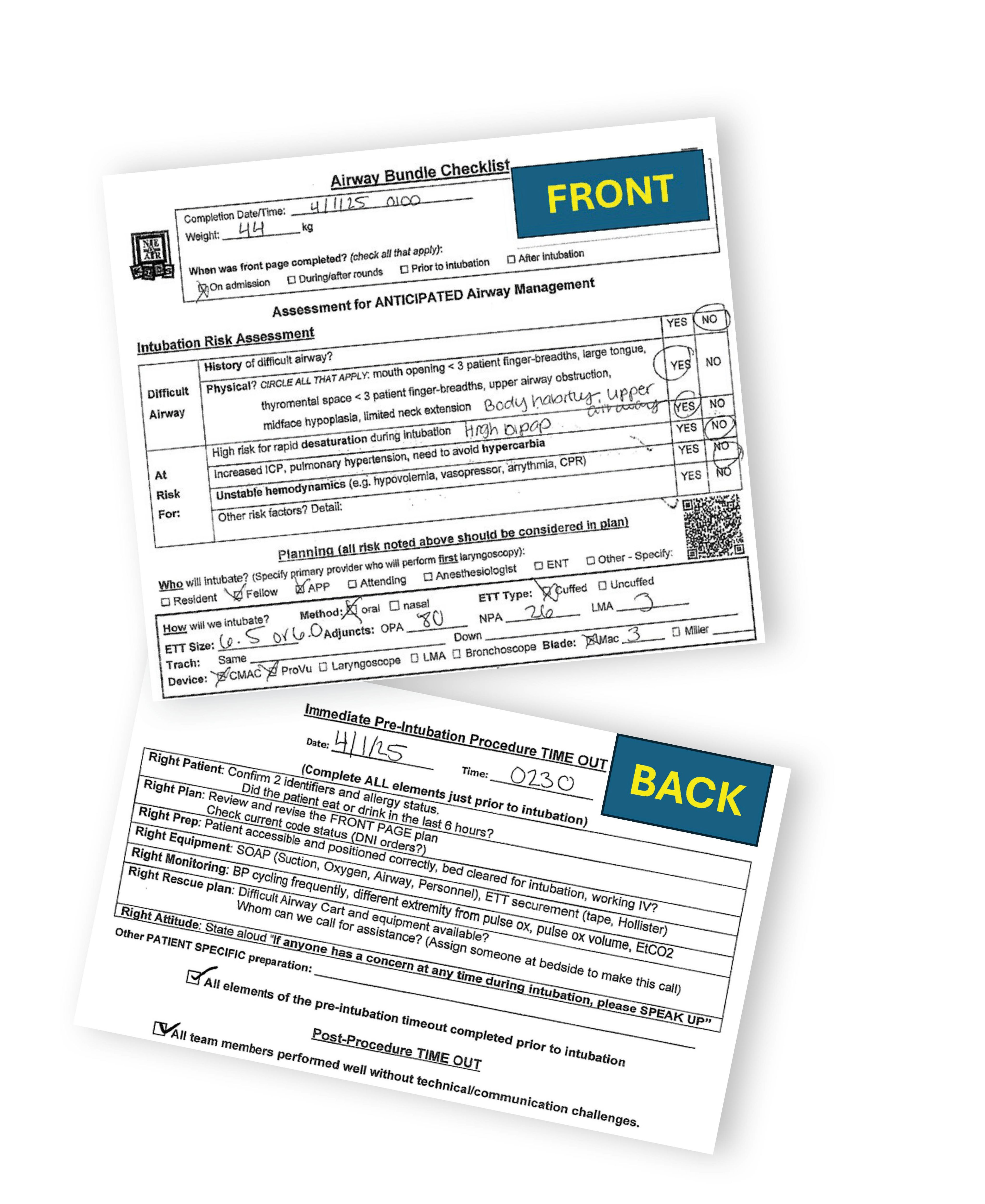
This journey began in 2018 when our team developed a pediatric Airway Bundle, a one-page tool designed to facilitate structured planning and team alignment around every intubation. The Bundle outlines individualized plans for medications, equipment and team roles based on the child’s airway history and clinical status. Using the Bundle standardizes care, reduces variability and ensures everyone is aligned before, during and after the procedure.
Introducing the Airway Bundle was a turning point in improving and standardizing intubation care. With consistent use and data tracking, Children’s Wisconsin was accepted into the National Emergency Airway Registry for Children (NEAR4KIDS) collaborative, a multicenter quality improvement initiative founded at Children’s Hospital of Philadelphia. This national registry tracks tracheal intubation-associated events (TIAEs) across more than 60 pediatric and cardiac ICUs globally, creating a powerful benchmarking tool to drive quality at the local level.
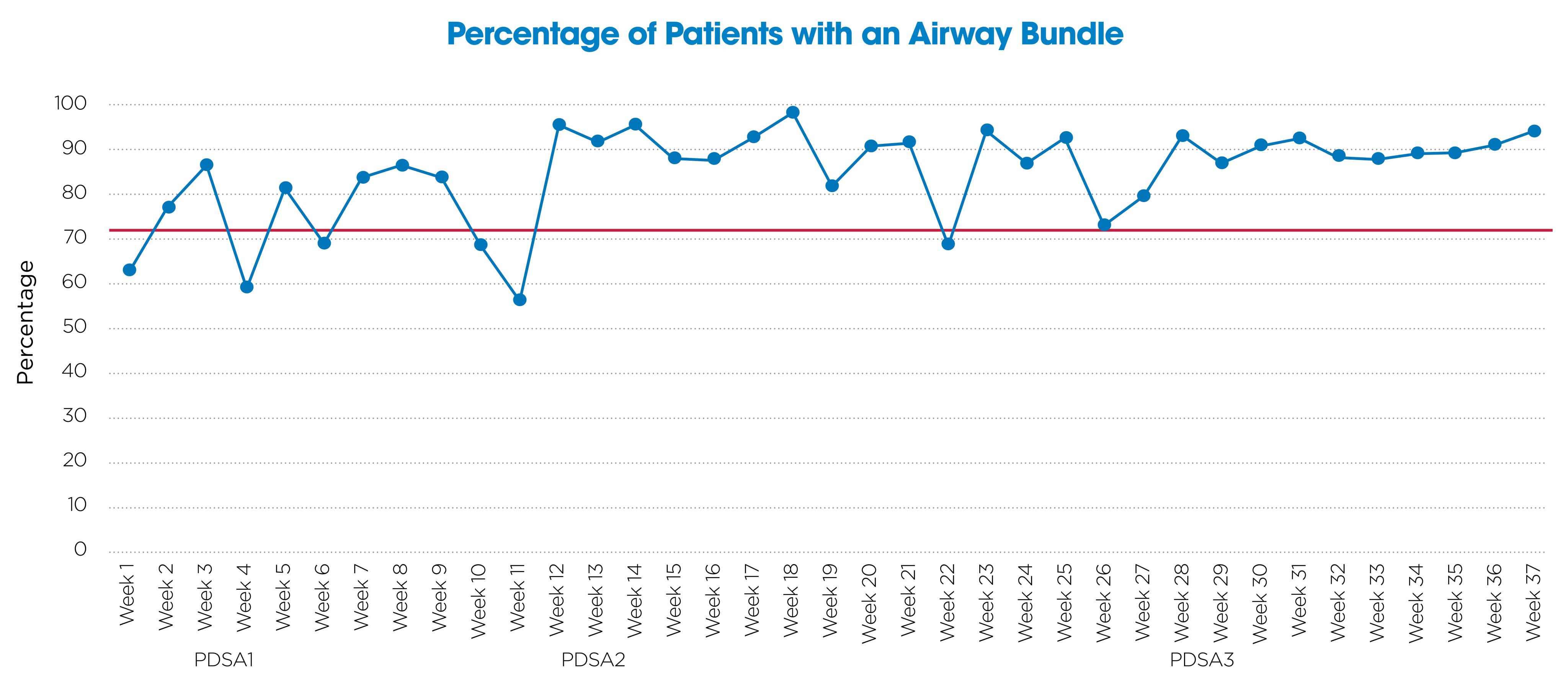
Our team’s initial focus was straightforward: Ensure every eligible patient in the PICU or CICU had a completed Airway Bundle within two hours of admission. We monitored and improved compliance through multiple Plan-Do-Study-Act (PDSA) cycles, eventually achieving and maintaining rates above the 70% target. By 2024, compliance stood at 87%, demonstrating our commitment to consistent, high-quality care.
As the reliability of the process increased, our team shifted focus to outcomes. National data from NEAR4KIDS reports an average TIAE rate of 20% during pediatric intubations.1 2 In 2018, the baseline rate at Children’s Wisconsin mirrored this at 22%. But through Bundle-driven planning, education and post-event debriefs, we steadily reduced this rate to 13.5% over successive PDSA cycles.
In 2023, we integrated airway safety work into the electronic health record (EHR), introducing standardized documentation templates for intubations. This innovation streamlined safety data collection, reinforced best practices and improved real-time visibility into a child’s airway history. The results were dramatic: TIAE rates dropped further to an average of 7.14%, significantly outperforming the NEAR4KIDS national average of 11.31% during the same period.
What makes the Children’s Wisconsin airway safety initiative stand out is not just the improvement in metrics but also the culture it has fostered. Every intubation includes a structured debrief section within the Bundle, creating space for immediate team reflection on what worked and what could improve. These debriefs are not punitive — they are tools for learning, feedback and evolution.
This feedback loop has become a valuable source of insight, helping identify recurring communication gaps, equipment issues and workflow inefficiencies. Plans are underway to analyze these findings in aggregate to enhance system-level planning and training.
While our current focus remains on PICU and CICU intubations, future plans include expanding the use of the Airway Bundle to intubations occurring in other care settings, such as the Emergency Department and operating rooms. Additionally, Bundle debrief data will be used to improve equipment access and team readiness, extending the same high-reliability practices across all high-risk environments in the hospital.
Ultimately, this initiative exemplifies what’s possible when data, teamwork and continuous learning converge. By leveraging clinical expertise, national benchmarking and real-time feedback, Children’s Wisconsin is not only improving care for today’s patients but also laying the groundwork for a safer, smarter future in pediatric critical care.
References
1. Parker MM, Nuthall G, Brown C 3rd, et al. Relationship Between Adverse Tracheal Intubation Associated Events and PICU Outcomes. Pediatr Crit Care Med. 2017;18(4):310-318. doi:10.1097/PCC.0000000000001074.
2. Colman N, Newman JW, Nishisaki A, et al. Translational Simulation Improves Compliance with the NEAR4KIDS Airway Safety Bundle in a Single-center PICU. Pediatr Qual Saf. 2021;6(3):e409. doi:10.1097/pq9.0000000000000409.